Ideas
India’s Malnutrition Problem Is Not Going Away Anytime Soon Despite Intervention
Ekta Chauhan
May 26, 2018, 01:24 PM | Updated 01:24 PM IST
Save & read from anywhere!
Bookmark stories for easy access on any device or the Swarajya app.


According to the latest UNICEF report, India was tenth in a list of countries with the highest number of underweight children, and seventeenth among countries with the highest number of stunted children. This is a huge problem, especially for a developing nation like ours whose demographic dividend is its biggest strength. At 356 million, India has the largest youth population in the world. But statistics suggest that the country is facing a substantial malnutrition problem despite its improving economic status in recent decades.
According to the Global Nutrition Report 2017, which looked at 140 countries, India has a twofold challenge – a large number of people are either underweight or overweight. Both these issues are linked to inadequate nutrition and unsuitable lifestyle.
The report especially highlights the “significant burden” of childhood stunting, anaemia in women of reproductive age, and overweight adult women. The 2017 figures show some worrying trends among women and children – 38 per cent of children under five are stunted (children whose height is below the average for their age), about 21 per cent of children under five are ‘wasted’ or ‘severely wasted’ (children whose weight is below the average for their age), 51 per cent of women in reproductive age suffer from anaemia, and 22 per cent of adult women are overweight.
Country prevalence estimate of stunting among children under age of five years (2011)
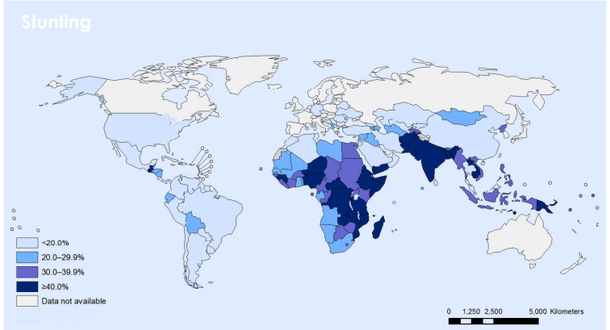
Even though the number of stunted children under five years of age in the world has declined from an estimated 253 million in 1990 to 165 million, the target of 40 per cent reduction in the global numbers by 2025 (since 2010) remains out of reach under current rates of decline. In addition, as one can see, there is a high disparity between nations with a high burden on South Asia (including India) and Africa.
District- and state-wise distribution of incidence of stunting among children (2015-16)
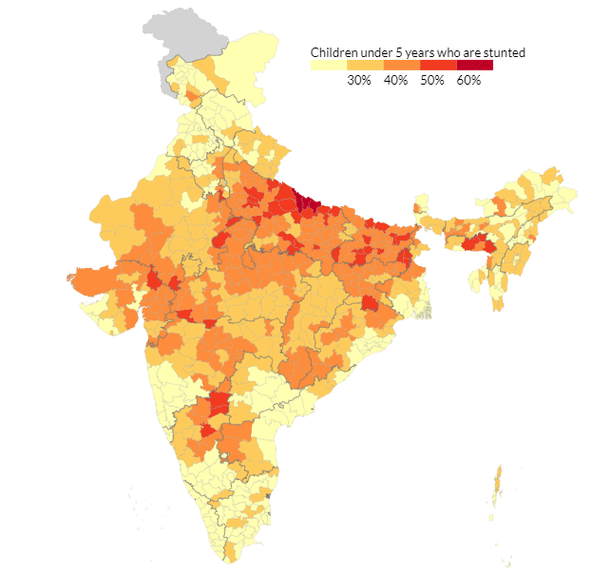
Even within India, a high disparity can be seen among states. While percentage of children suffering from stunting is under 30 per cent for states like Kerala and Tamil Nadu, it is as high as 50 per cent in states like Bihar and Madhya Pradesh.
The report also highlights that while India has improved in addressing the problem of stunting in children under five years, it has made no progress or even presents worse outcomes in the percentage of women in the reproductive age with anaemia, and is off track in terms of targets for reducing adult obesity and diabetes. The twin challenges of the weight being lower or higher than the average, presents a unique challenge for the country and highlights the growing gap among social groups and their respective lifestyles. It is a well-established fact that healthier kids grow into productive adults and thus contribute positively to the economy. Lack of nutrition actually reinforces the cycle of poverty.
Similarly, the health of the mother has significant and lasting impact on children, especially the girl child. According to UNICEF, “Undernourished girls have a greater likelihood of becoming undernourished mothers who in turn have a greater chance of giving birth to low birth weight babies, perpetuating an intergenerational cycle. This cycle can be compounded further in young mothers, especially adolescent girls who begin childbearing before they have grown and developed enough. When mothers take only short intervals between pregnancies and have many children, this can exacerbate nutrition deficits, which are then passed on to their children”.
As the World Nutrition report also highlights, India is one of the worst performers in women’s health. According to the WHO, India comes at the bottom of the table with 51 per cent women suffering from anaemia. The first four countries are China, Pakistan, Nigeria, and Indonesia. Anaemia is a serious condition that can have long-term health impact for mother and child. UNICEF data suggests that a third of the women of reproductive age in India are undernourished, with a body-mass index of less than 18.5 kilogram per metre squared.
What is the state doing?
While addressing the problem is complex due to the many factors involved, governments have been trying to improve things. Several schemes such as the Integrated Child Development Services, the National Health Mission, the Janani Suraksha Yojana, the Matritva Sahyog Yojana, the Mid-Day Meal Scheme, and the National Food Security Mission are in operation at the grassroots level. The Modi government also launched the National Nutrition Mission in 2017 with an aim to reduce all forms of malnutrition by 2030, and a focus on the most vulnerable and critical age groups. The strategy also aims to assist in achieving the targets identified as part of the Sustainable Development Goals, to which India is a signatory, related to nutrition and health. Among the highlights of the policy are its decentralised approach, introduction of specific interventions with a focus on improving healthcare and nutrition among children, measures to improve maternal care and nutrition, and governance reforms.
As is the case with any human health-related problem, the gestation period for any policy is high. While the National Nutrition Mission is a step in the right direction, it will take years before one can see noticeable change in the current (dismal) state of the health of our mother and children.
Road ahead
While the government has put nutrition at the heart of its health policy, more needs to be done. One of the ways to improve nutrition intake among kids is to deliver supplements through self-help groups as well as include them in mid-day meals. Diversifying the current Public Distribution System (PDS) can be another important step. While the programme has been beneficial in providing food to the poor, it is currently limited to only wheat and rice (among grains). Millets and coarse grains are rich in micro-nutrients and fibre content, and bringing them into the PDS fold can positively change the consumption pattern of the poor. This would, in addition, also increase the income of farmers who grow coarse grains.
Awareness and knowledge campaigns among mothers and pregnant women can be a great way to sensitise them about the importance of a healthy diet. Even if knowledge campaigns don’t lead to behavioural changes immediately, and such changes may be affected by other social and economic factors, knowledge in itself is necessary is further steps are to be taken.
More importantly, states need to improve investment in social welfare. In a paper titled ‘Child Development Index: How Have Different States Fared’, economists Reetika Khera and Jean Dreze analyse the key reasons for the rapid progress made by Kerala, Tamil Nadu, and Himachal Pradesh in improving their nutrition indicators. They found it was a significant expansion of elementary education and of essential services and facilities, from healthcare and clean water to social security, and providing a voice to the disadvantaged groups, that worked in these states. Perhaps this is the way to go in other states as well.
Ekta is a staff writer at Swarajya.




