Infrastructure
Why Family Caregivers Need A Hand To Hold
Swati Kamal
Feb 27, 2019, 06:18 PM | Updated 06:18 PM IST
Save & read from anywhere!
Bookmark stories for easy access on any device or the Swarajya app.
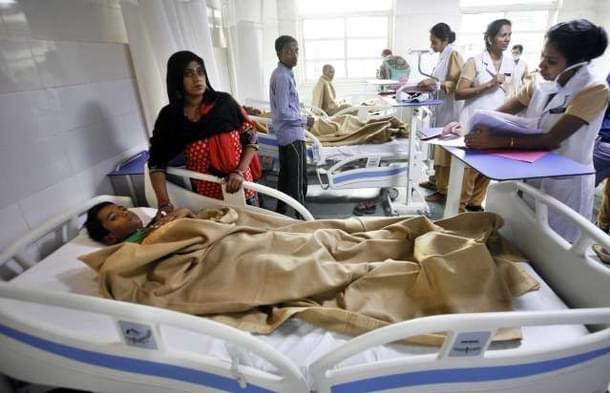

When Kumud Kalia’s husband was diagnosed with the rare disease, Shy-Drager syndrome, with no known cure, she experienced a plethora of emotions. “I was numb initially, and then I wanted to hide. I felt I could fight it and was determined to cure him. Acceptance came over time, but the anxiety never left. I wanted to do everything myself and did not want to take help. I also became very bitter with people who I felt did not empathise enough, and the result was withdrawal and social isolation. I felt guilty taking a break and going out, even though it did provide relief. The emotions are so high that you cannot talk about it, and people are also wary of approaching you. Yet, each time I was offered help, I was grateful”.
“The truth is, the person taking care of terminally ill patients gets so depleted that they are also sick and require a different kind of hand-holding. In our family systems, the patient is taken care of, but the care givers neglected themselves and are also neglected by the community.”
The little bit of empathy reserved for caregivers is visible outside the Basavatarakam Indo-American Cancer Hospital in Hyderabad. Here, one sees people, who emerge from the makeshift housing, basic tents, forming large queues at certain times of the day. The kith and kin of cancer patients undergoing treatment inhabit these tents, and they queue up for food that is cooked and brought in vehicles by Samaritans. This food 'seva’ is routine in the cancer hospital, prompted by a feeling that “it is the least we can do”.
This help, though indispensable, is actually a drop in the ocean of the challenging life of a caregiver. The surgery or emergency that brought them to the hospital would inevitably pass; but the care and responsibility are lifelong, when dealing with patients afflicted with chronic diseases.
In India, this caring and tending has been traditionally handled by family members who consider it their duty. But what has traditionally been the strength of the Indian system, is getting weakened by increasing urbanisation, fragmentation of communities and the phenomenon of nuclear and small family units. With a hectic pace of life, distractions that abound, limited attention spans and a generally declining lack of concern, what was earlier shared across the community and extended family is now almost singularly handled by the primary caregiver.
“Urban stress is currently very high. For a caregiver, the stress is a few notches higher. This results in caregiver burden and caregiver depression and loneliness,” says Bhavana Issar, CEO and founder of CaregiverSaathi.
CaregiverSaathi is a Mumbai-based organisation that is in the process of creating an ecosystem of support for caregivers. Their programme is designed for caregivers in terminal illnesses and chronic conditions like cancer; neurological conditions like ALS (amyotrophic lateral sclerosis), MSA (multiple system atrophy), MS (multiple sclerosis); and mental health disorders like depression, schizophrenia, bipolar, Alzheimer’s, dementia, etc. They also cater to caregivers attending geriatric (ageing) and genetic conditions.
Bhavana saw at close quarters the herculean efforts that go into care-giving for the terminally ill, as her mother looked after her terminally-ill father. Eight years ago, this XLRI alumnus – who is passionate about motorcycles, crochet and poetry – finally realised this was actually her calling, after meditation on the full-moon night of Buddha Purnima.
She spoke to Swarajya on some issues surrounding this new emerging area in healthcare.
The Mindset Of Primary Caregivers
“The caregiver also needs care, emotional support, guidance from experts and wisdom from experience, knowledge and good judgement. The first step is to organise yourself to create the time and space for self-care.
“When care-giving falls into your lap – often unannounced – remember that you cannot care for someone meaningfully unless there is discipline of looking after yourself. Compassionate people become caregivers, but prolonged period of life-sucking circumstances can lead to `compassion fatigue’.
“Of late, there is so much spoken about `positive psychology’ – which really takes away the right of a person to experience feelings like frustration, anger, etc, which caregivers do tend to feel, towards the patient, towards themselves, towards the world and towards god. Caregivers need to know that it is common, and alright to feel this way.
“An interesting phenomenon is that we have moved from traditional medicine and healing practices that were holistic, to curative and intervention-based healthcare, over the last century. There is a kind of pressure on the caregiver/family member to extend life without necessarily looking at the quality of life.”
Exact Needs Of Caregivers
Bhavana laid down the five critical areas where caregivers find themselves struggling.
* Self-care versus patient-care
* Who can I talk to, who will understand me?
* Can I bring my challenges to the workplace?
* Do I do everything myself or can I get it done from someone?
* How can I get information for quick decision-making?
What follows these critical questions are more questions about funding of medical expenses, about the continuity or return to a job etc.
Bhavana said that the needs of caregivers vary, depending on the social strata, gender, education, life-stages of the caregiver and the care-receiver, the phase of care-giving, and individual circumstances. “We work with caregivers to develop their unique plan for seven aspects of well-being generally: physiological, financial/legal, psychological, social, life and work purpose, creative expression and spiritual well-being”, she said.
Challenges In This Barely Recognised Area Of Well-being
The biggest challenge according to Bhavana is convincing caregivers that they need help. Most people do not even recognise themselves as `caregivers’ because of the sentiments associated with the relationship. Then, they tend to deprioritise their own needs.
She adds: “Once they recognise their needs, they can work to help themselves. Care-giving to a dear one facing terminal illness or a chronic condition is a traumatic journey. But importantly, the healing of the patient hinges upon the caregiver's well-being.”
So CaregiverSaathi works with influencers of caregivers – employers, doctors, well-wishers, and so on. They try to create awareness and sensitivity through workplace workshops, community clubs, educational institutions, hospitals, doctors and health professionals, etc. Bhavana says: “To build this ecosystem, we need to get this need into the mainstream narrative. We then service it digitally, in-person or through workshops. So far we have a good response, especially in Bhakti Vedanta hospital in Mumbai and Hinduja Hospital.”
Tools And Techniques Used
Practices and knowledge bases like yoga therapy, psychological therapies, art therapy, group therapy are applied. Most of their programmes are designed using approaches adapted from systems thinking, design thinking and gestalt.
Ensuring This Support Is Available To The Last-Mile Person
To a lot of people the idea of caring for caregivers hits very close home because everyone has either seen caregivers in their family or been one. But despite recognition of this need, people may still be willing to pay for it.
Bhavana explains their business model and says, “Given that care-giving cuts across all sections of society, we would want our services to reach as many irrespective of their ability to pay for the services. Yet, we are not a philanthropic or charitable organisation. Though wealth creation and a business proposition are not the starting point for social innovation, they are still critical for sustenance. We need the support of all stakeholders, including philanthropists who are willing to back a venture that wishes to change the paradigm of healing and well-being.”
She adds, “This idea is not mainstream health, but it increases well-being in society. The government must give it priority. Perhaps, consider making it a part of general healthcare programmes like Ayushman Bharat. Currently, palliative care is included in Ayushman Bharat, but the scope of that must be increased to involve care-giving. Also, the medical system must also change the definition of palliative care – from end-of-life care, to a holistic system that improves the quality of life, right from the time of diagnosis.”
Government support would immensely help scaling up the programmes of CaregiverSaathi. Healthcare professionals across categories could be given training in caregiver sensitivity and palliative care. Of course, in a large complex country like ours where issues like polio, maternal health and infant mortality are in the forefront, this area is still not priority. But there is a crying need for it.
Bhavana concludes, “Countries like the US, the UK, Canada and to some extent, Australia and New Zealand have organisations that support caregivers. We draw our inspiration from many of them and are in conversation with some of them to build partnerships and alliances. The governments and the healthcare systems stand to benefit by looking at this critical constituency.”
Policy Perspectives
With society seeing an increasing number of chronic and terminal illnesses such as cancer, autoimmune disorders, neurological conditions, diagnosed mental health conditions like Alzheimer’s, dementia, genetic conditions and also an ageing population, every other family now has one kind of patient or another. Ergo, large numbers of caregivers in the country.
High caregiver stress levels would inevitably lead to dysfunctionalities in various spheres of life, impacting daily living, relationships and so on.
In a 2016 paper in the Indian Journal of Social Psychiatry, 'Care-giving and caregivers: Challenges and opportunities in India', author R S Murthy, who works closely with cancer patients and their families, argued that family caregivers need to be supported and nurtured through programmes of information and practical assistance. He emphasises that “for healthcare in general and mental health and chronic illness care in particular, there is an urgent need to fully understand the care-giving in different communities, population groups, and develop programmes to make care-giving a positive experience.”
The Economic Survey 2019 is reportedly going to include some off-the-beaten-track parameters like mapping India in relation to its demography, habits, nutrition, inequality, break up of major disease patterns as also claims patterns of Ayushman Bharat – all towards chalking out future policies and programmes.
This area needs national attention. A good starting point could be taking a leaf from the US, where laws are being passed that will require hospitals to figure out who a patient’s caregiver is and attach that information to the patient's hospital record. That allows health systems to support caregivers directly.
For the sake of the collective sanity and well-being – and for the sake of true universal health coverage – we must do it.
Swati Kamal is a columnist for Swarajya.





